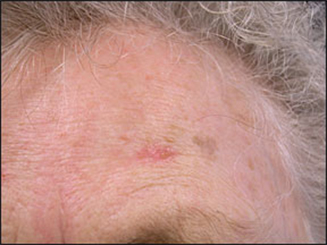
Actinic keratosis (AKs) is known as the early beginnings of skin cancer. This most common lesion of the outermost layer of the skin (epidermis) is caused by long-term exposure to sunlight (specifically to ultraviolet wavelengths). AKs are most likely to appear after age 40-50, and years of chronic exposure to the sun. However, in geographic areas with year-round high-intensity sunlight (e.g., Florida, southern California). AKs are now found in persons as young as the teens and twenties. The incidence of AKs is over 50 percent in older, fair-skinned persons in hot, sunny geographic areas.
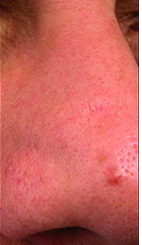
II. DEFINITION:
II. Actinic Keratosis Causes: AKs are defined as a cutaneous dysplasia skin growth of the epidermis (the outermost layer of skin). In everyday terms, AKs are an alteration in size, shape and organization of skin cells. The cells most affected in AKs are the keratinocytes, the tough-walled cells that make up more than 90 percent of the epidermis and give the skin its texture. Cellular alterations in AKs may extend into the dermis, the layer of skin under the epidermis. The most significant cause of actinic keratoses is long-term exposure to sunlight, and specifically to the ultraviolet wavelengths of solar radiation. The most significant predisposing factor to AKs is fair skin.
The alteration in skin growth and differentiation of keratinocytes is manifested in the clinical features of AKs - rough, scaly skin, "bumps" on the skin, mottled skin, and cutaneous horn. Alterations in cell growth and differentiation also set the stage for transformation of AKs into invasive squamous cell carcinoma.
Cryosurgery:
Liquid nitrogen "freezes" surface skin, which subsequently flakes off to be replaced by new skin. Skin redness for a time is the chief side effect. Cryosurgery is one of the most commonly used treatments, especially by dermatologists.
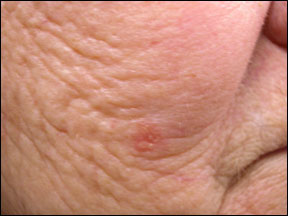
Shave Excision:
Shave excision usually removes the actinic keratosis with the most precision. A specimen can also be sent to a pathologist to confirm the diagnosis (since it is not destroyed like in cryosurgery). Skin redness for a time is the chief side effect. Shave excision is one of the most commonly used treatments, especially by plastic surgeons. The cosmetic result is usually better than that achieved by other methods of removal.
Surgical excisional biopsy
Actinic keratoses are surgically removed with an excisional biposy and the tissue examined under a microscope when there is suspected transformation into invasive squamous cell carcinoma.
Topical and systemic retinoids
Retinoids (vitamin A derivatives) are potent agents that can normalize abnormal growth and differentiation in keratinocytes. They must be prescribed by a doctor after full dermatologic and medical examination, and their use must be monitored regularly. Retinoids have a number of side effects, but skin irritation is the most common.
Topical chemotherapy
A topical anti-cancer agent (e.g., 5-fluoruracil) is applied to the skin to remove actinic keratoses lesions. A localized red spot may remain for some time at the site of chemotherapy application.
Chemical peel
In a chemical peeling treatment, a chemical solution is applied to the skin causing the skin to blister and peel off over a period of days. As the treated skin blisters and peels, new skin forms to replace it. Your plastic surgeon will select a chemical solution to accomplish a mild, medium or deep peel. The principal side effect is redness and swelling of skin for a period of time after the treatment.
Dermabrasion
Skin is abraded away with a rapidly rotating brush, down to the depth necessary to remove sun-damaged skin. New skin grows to replace the removed, damaged skin. Redness of skin and some discomfort are the chief side effects, usually resolving within 10 days. Your plastic surgeon can relieve the side effects with medications.
Laser skin resurfacing
A series of treatments with the carbon dioxide or erbium laser removes surface skin to a desired depth. Post-treatment skin redness is the principal side effect. A week or two of healing is needed.
Electrosurgical skin resurfacing
A pulse of electromagnetic energy at radio frequency removes surface skin. Mild to moderate post-treatment swelling is the chief side effect.
Actinic Keratosis Picture Treatment should be fully and openly discussed with your plastic
surgeon. After actinic keratoses are removed, the new skin must be protected from new solar damage by a regimen of skin care that includes sun protection and regular use of moisturizers.

47 year old female before and 5 months after shave excision of right for head actinic keratosis. This is a pre-cancer. About 10-15% of these will become squamous cell skin cancer within 5 years. Patients have the option to formally excise these areas if they are worried but in the majority of them, we just observe them to see if anything ever comes back or a new lesion arises. Patient also started using our Scar Support Product two weeks after her procedure. She did not have any laser treatments.
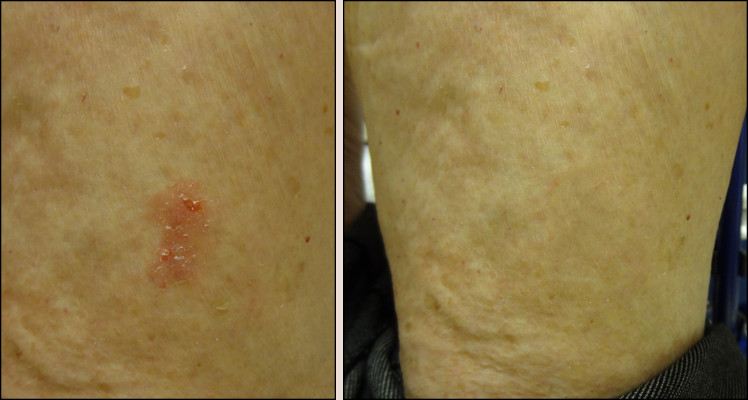
82 year old female before and 8 months after shave biopsy of a left thigh actinic keratosis. A biopsy will help us determine if this is skin cancer. If the pathology results come back as actinic keratosis (precancerous), most patients opt to just observe this rather than cut it out which is reasonable. 85% of the time no lesion recurs. If the pathology report shows actinic keratosis with bowenoid features, this is further along on the spectrum and usually excision is recommended for these. She did not have any other treatments.
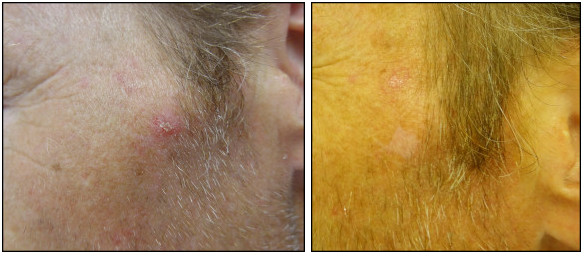
52 year old male before and 1 month after shave excision of left zygoma actinic keratosis. This healing well and patient did not want any other treatments.
When I first published The 7 Critical Questions to Ask Before Letting Any Surgeon Touch You, I had no idea that it would be so popularly received. Since its publication, this brief guide has helped thousands like you to more safely navigate the world of cosmetic surgery. The 7 Questions have been updated and a bonus section, Applying the 7 Questions, has just been added. Be my guest to read, learn and share.